3 Drivers of Opioid Dependence
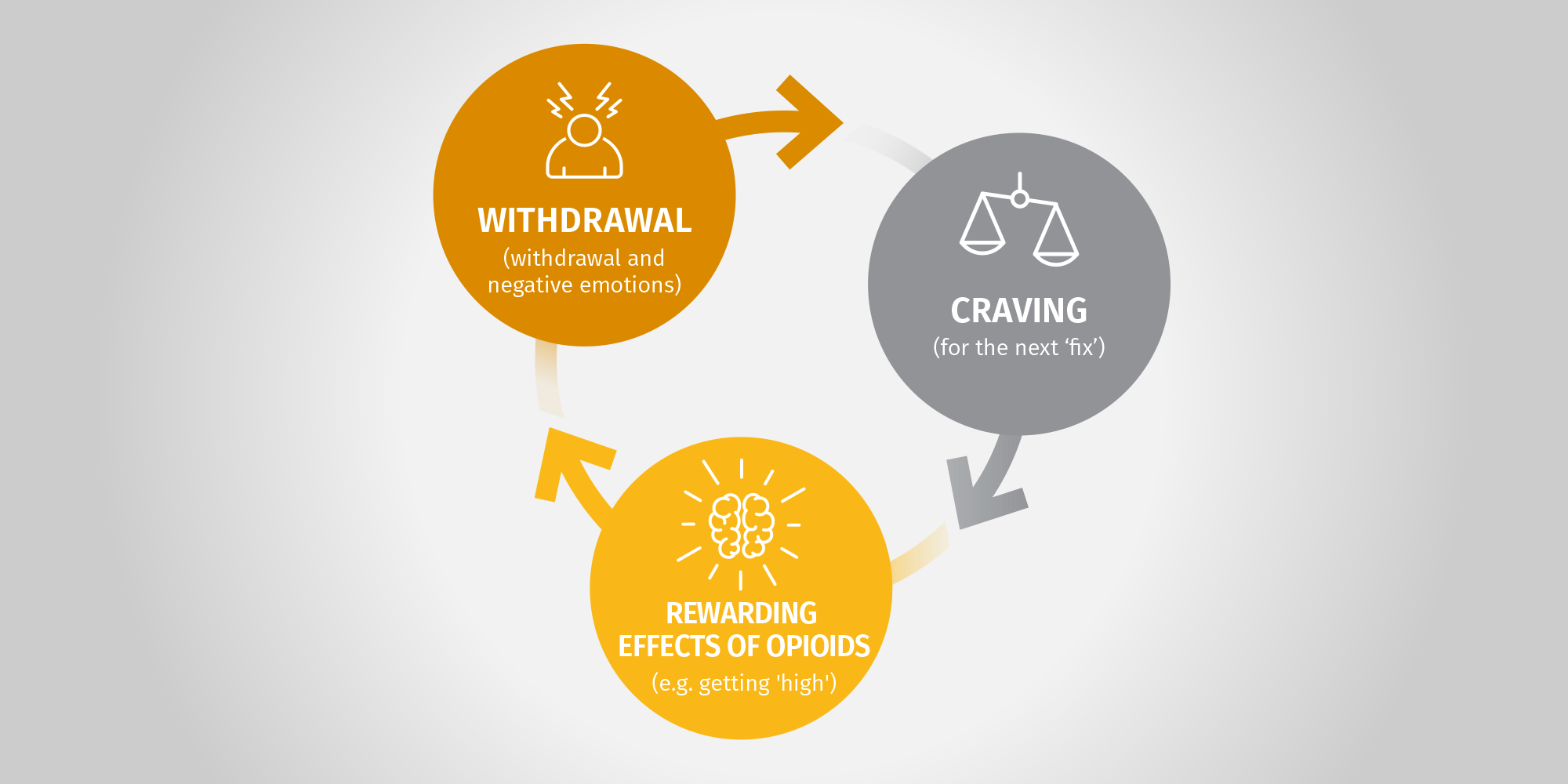
Opioid dependence is a chronic, relapsing disease caused by opioids altering the brain’s neurobiology and changing the way someone thinks, feels and behaves.1,2 The 3 drivers, the rewarding effects of opioids, withdrawal and craving, feed into one another to drive the cycle of opioid dependence and become more intense over time.3
The cycle of opioid dependence
Initially, people take opioids to simply feel their rewarding effects. Over time, with continued use, this changes and people may find that they can only function ‘normally’ when the opioid is present. Without opioids, they experience withdrawal – one of the most-powerful factors driving opioid dependence. The more someone uses, the more they crave the opioid when it’s not there.3 And so, the cycle continues. It’s no wonder that opioid dependence can be a difficult cycle to break.
So, how exactly does each driver work to drive the cycle of opioid dependence?
Opioids cause a large increase in dopamine and activate the basal ganglia, leading to feelings of euphoria.1,4 With repeated use, the brain learns to associate taking the opioid with the reward response. However, unlike ‘natural rewards’ such as food or sex, opioids do not lead to the feeling of being full or satisfied. People never feel like they’ve had enough and instead, continue to use opioids. This can result in heavy or ‘binge’ use of opioids.1,2
Over time and with repeated use, the extended amygdala becomes less sensitive to the opioid.2,4 People become more sensitive to stress and as the opioid effects wear off, withdrawal symptoms emerge and if not properly managed, can sometimes be fatal.2,5 Withdrawal can be extremely uncomfortable (e.g., diarrhoea and vomiting, sleep problems, and muscle and bone pain)5,6 and further drives opioid use to prevent the distressing symptoms.
Changes occur in the prefrontal cortex, which is involved in decision making, impulse control and emotions.1,4 Defined as an overwhelmingly strong desire or need to use an opioid, craving can dominate a person’s thoughts and become all-consuming.7,8 As a key motivational driver in opioid dependence, craving is reflective of a learned association between withdrawal relief and opioid-drug taking.8,9
Treating opioid dependence
Breaking this cycle requires more than just willpower.
Like diabetes, heart disease and other chronic conditions, opioid dependence is an illness that requires treatment. What’s more is that opioid dependence is not a standalone disease and is usually accompanied by psychological and social issues, which can be both the underlying reasons for opioid use and the result of using opioids. Knowing this, a combination of medications and psychosocial support is essential to break the cycle of opioid dependence.5 
Medications such as methadone and buprenorphine for medication-assisted treatment, work by addressing the 3 drivers of opioid dependence and lead to the:5
• Reduction of the physical withdrawal symptoms
• Suppression of cravings
• Blockade of the rewarding effects of opioids
Counselling is an important component of treatment for opioid dependence as it helps people recognise situations, feelings or events that could ‘trigger’ a desire to use opioids and teaches them new coping skills to avoid or manage these triggers.5
Relapse from treatment is a common experience and should not be viewed negatively. Relapse-prevention treatment aims to reduce opioid use and commonly involves a combination of an antagonist (e.g., naltrexone) and counselling. Coping strategies and skills will also help people avoid and deal with high-risk situations.5,10
By understanding how the 3 drivers work and knowing the treatment options available, it’s clear that opioid dependence is a treatable condition and not a moral failing.11 As a healthcare professional, connecting patients with treatment is essential to help them overcome their opioid dependence.
If you would like to learn more about breaking the cycle of opioid dependence, visit the TurntoHelp website for healthcare professionals.
References:
1. Volkow ND, et al. N Engl J Med. 2016;374(4):363–371.
2. Koob GF and Volkow ND. Neuropsychopharmacology. 2010;35(1):217–238.
3. Kosten TR, George TP. Sci Pract Perspect. 2002;1(1):13–20.
4. Substance Abuse and Mental Health Services Administration (US); Office of the Surgeon General (US). Facing addiction in America: The Surgeon General’s report on alcohol, drugs and health. 2016.
5. Gowing L, et al. National guidelines for medication-assisted treatment of opioid dependence. Australian National Drug Strategy. 2014.
6. National Institute on Drug Abuse. Prescription opioids drugfacts. 2021. Available at: https://nida.nih.gov/publications/drugfacts/prescription-opioids (accessed 23 February 2022).
7. Kakko J, et al. Front Psychiatry. 2019;10:592.
8. Tiffany ST and Wray JM. Ann N Y Acad Sci. 2012;1248:1–17.
9. Koob G. Biol Psychiatry. 2020;87(1):44–53.
10. Department of Health. 8.1 Relapse prevention/management. 2004. Available at: https://www1.health.gov.au/internet/publications/publishing.nsf/Content/drugtreat-pubs-front9-wk-toc~drugtreat-pubs-front9-wk-secb~drugtreat-pubs-front9-wk-secb-8~drugtreat-pubs-front9-wk-secb-8-1#rel (accessed 24 February 2022).
11. Matano RA and Wanat SF. West J Med. 2000;172(1):63.



